HIGH POINT, N.C. — In the 15 minutes it takes to read about a High Point family's harrowing journey with a cruel illness, one more child in America will receive the life-changing diagnosis affecting 40,000 babies in the U.S. each year -- Congenital Heart Defect (CHD).
The prevalence of the wide-ranging illness is why, during this National Heart Month of February, the Rosses share their emotional CHD journey – from heartbreak to healing…and hope.
Caleb’s Story
High Point mother and teacher Amy Ross often hears her thoughts take the tune of a favorite hymn:
When peace like a river, attendeth my way… /
When sorrows like sea billows roll; /
Whatever my lot, though hast taught me to say... /
“It is well, it is well with my soul.”
The Biblical passage from which it derives is how Ross describes a soul-searching journey, chronicled straight from the heart.
“I would hear things, and immediately go type, because I didn’t want to forget,” she said.
Ross began blogging in late 2020, when she, husband Adam, and son Aaron learned their family was growing.
“I remember taking a pregnancy test and the line popping up immediately,” Amy Ross recalled.
Adam Ross added, “It happened so fast… when she’s like, 'Oh, you know, I’m pregnant,' I was like, ‘Whoa!’ It was nuts.”
However, in a heartbeat, the tide turned, as their story’s next entry transcribed a test of faith. Amy Ross went to her 20-week anatomy ultrasound (solo, because of COVID protocols at doctors’ offices at the time) and was nervously excited to mark the halfway point of her pregnancy.
“Initially, in the ultrasound, everything looked good, everything looked fine, but I know when I was in the waiting room waiting to speak to the doctor, I was waiting a little while,” she recalled.
The scan had revealed an abnormality – a Congenital Heart Defect, known commonly by its acronym CHD.

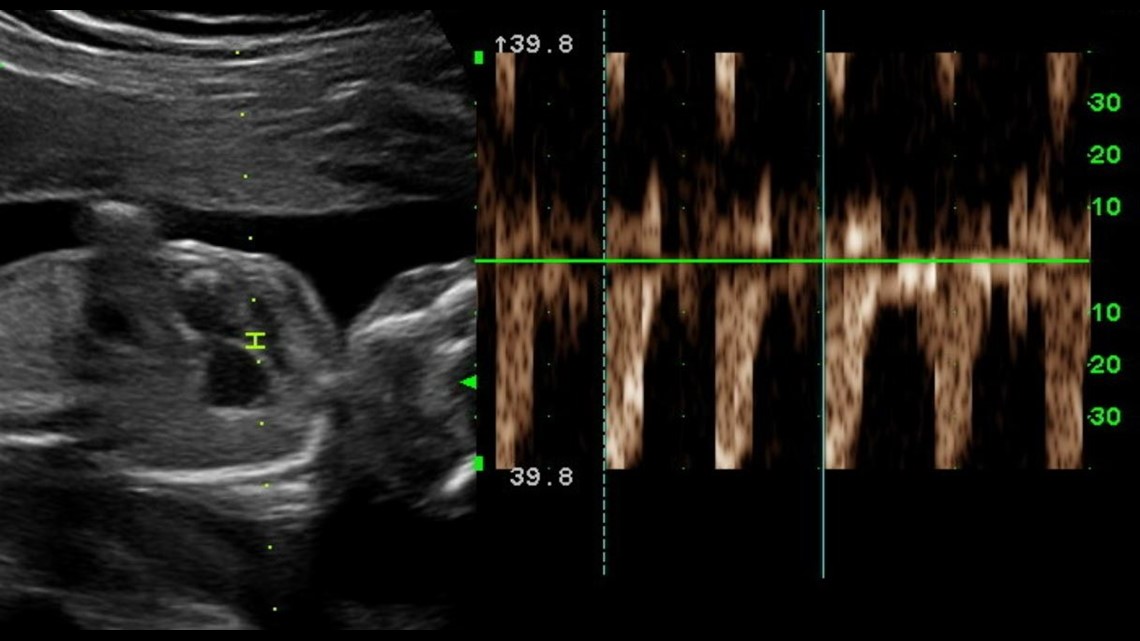
“I knew with the steps going forward, I would have to be strong,” admitted Adam Ross.
The case came to Atrium Health Wake Forest Baptist, where fetal and pediatric cardiologist Michael Walsh, MD, determined Baby Ross had evolving Hypoplastic Left Heart Syndrome (HLHS) – a faulty left side.
“The first thing we noticed was one of the pumping chambers, specifically the left ventricle was not doing what it was supposed to do. It was extensively scarred, and it wasn’t squeezing like it should be,” said Walsh.
He later confirmed Caleb’s CHD had evolved to include a Restrictive Atrial Septum (RAS) – limiting blood flow between the heart’s top chambers.
“If that pathway is obstructed for blood to exit the lungs, then that blood backs up in the lungs,” he explained.
Baby Ross’s diagnoses are among the quarter of all CHDs considered, by the Centers for Disease Control and Prevention, to be critical – requiring surgical intervention for survival.
“We do believe that long-term outcomes, especially from a neurological and cognitive side, will be improved if we can make it to term. But, not all babies allow us to wait that long,” explained Walsh.
Two weeks before a scheduled 35-week delivery at Levine Children’s Hospital in Charlotte, where the Rosses just had left a consultation, the baby flipped the script – too early.
“It felt like we were home for five minutes, and her water broke,” Adam Ross recalled.
They rushed back and prepped for a cesarean delivery, leaning on prayer and each other.
“I remember trying to calm him (Adam), and I said, ‘Look at all these angels God has brought to surround us right now,'” Amy Ross reflected emotionally, about the doctors and nurses in the operating room.
With comfort and courage, Amy Ross delivered her four-pound baby boy, named Caleb.

“Caleb means wholehearted and bold and brave; his heart was half of a heart, and we were in this journey to make a whole heart,” Amy Ross smiled.
That journey began immediately, as physicians wheeled Caleb away to his first heart surgery.
“The intervention he had in the cath (catheterization) lab was to help stabilize him and help him to eventually grow to reach a bigger size for the next intervention,” explained Levine pediatric critical care physician Jennifer Bailey, MD.
Bailey noted Caleb’s prematurity, coupled with the development of RAS, upped the risks.
“He developed some significant complications from that procedure and actually had a cardiac arrest, where he needed CPR briefly and another emergent procedure for developing some fluid around the heart,” she explained.
For the next week, Caleb fought hard, giving glimpses of hope – like when he opened his eyes to the sound of his parents’ voices. His story was writing a new beginning, until suddenly – the words stopped.
“On the day we went in (to the NICU) to…just visit and get some answers about future physical therapy and all of that, Dr. Bailey comes in and says, ‘We have to share some difficult news with you. There has been a massive, massive brain bleed,'” Amy Ross said.
Dr. Bailey explained, “That (the brain bleed) put him in a risk category that would not allow him to have any other cardiac interventions or any life-saving medications.”
No future option to fix his heart meant no chance Caleb could survive.
“The world started spinning,” Amy Ross recalled.


First hellos became last goodbyes, and eight days after Caleb entered the world in pain, he left it in peace – in his parents’ embrace.
“We sat and held him and he had no wires, he had no tubes, and (it was) the first time seeing your little boy without all of these things that were keeping him alive, and to see his little face…and spend those last moments with him and be able to hand him over to God,” Amy Ross cried.
Studying Special Hearts
Caleb and 40,000 other heart warriors born in America each year are the ‘heartbeat’ of ongoing research, like the North Carolina CHD Network’s new database to learn causes and find cures. Atrium Health Wake Forest Baptist and Atrium Health Levine Children’s are two of the seven NC hospital systems working together on the surveillance.
“Our center is in the process of collecting data on race and ethnicity, and we hope to get some very good data on that,” explained Bailey.
Researchers also are looking at disparities in boys versus girls, as well as genetic links. The Children’s Heart Foundation reports most CHDs (like Caleb’s) have no known family history. That is why physicians, researchers, and parents advocate for more research funding to pinpoint risks and improve interventions, even in pregnancy.
“We expect in 10 to 20 years from now, the discussions we have with our families may be very different from the discussions we have with them now, and that’s very exciting," Walsh said.
Finding Strength in Faith
The prospect of hope for better CHD outcomes is the theme of Caleb’s heart story, as his mother – two years later – writes the epilogue.
“Just getting to say he was alive, he lived, and he means something – (it matters) not just to us but to others, as well, so spreading awareness is such an important thing for us,” Amy Ross emphasized.
She credits her strength in faith...to a messenger from God, appropriately named Gabriel – Caleb’s twin.
Yes, the entire time, there were two hearts beating as one – a brotherly bond unbroken by loss.

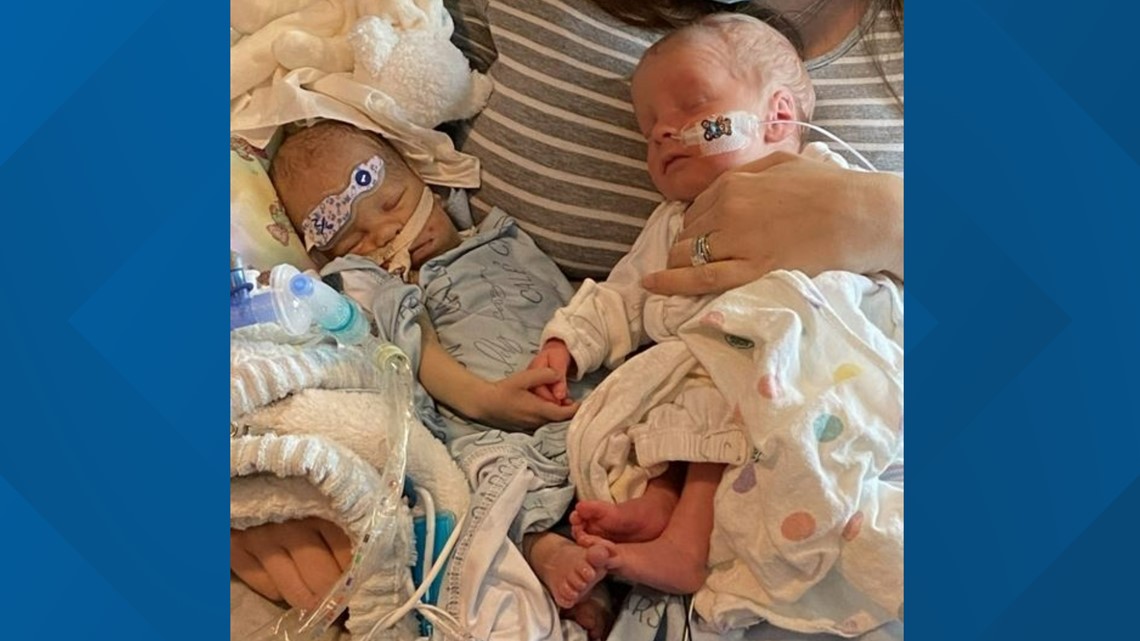
“There are a lot of times I look at him (Gabriel), and I think, ‘You’re a twin. You have a brother,’ and we have to keep his memory alive because that is a relationship he didn’t get to experience here on earth,” Amy Ross explained.
She said on particularly-emotional days, like the boys’ birthday and the anniversary of Caleb’s passing, she again draws strength from the words of a comforting hymn:
“…It is well, it is well with my soul.”
“Our soul is one of those things you have to work on all the time. It’s not easy every day… you learn to accept this is a purpose for us, this is our story, and we need to use it for good. We’ve found a lot of peace knowing he (Caleb) is OK, he’s healed, and we will see him one day again,” she smiled.
Until that day comes, the Ross family vows to love, like Caleb, “wholeheartedly.”
Supporting Heart Families
As Amy Ross begins to share her family's CHD journey more publicly, she hopes to be a mentor to other parents whose children have CHDs. She encourages and appreciates support for the medical centers and non-profit agencies advocating for heart families, like hers, every day.