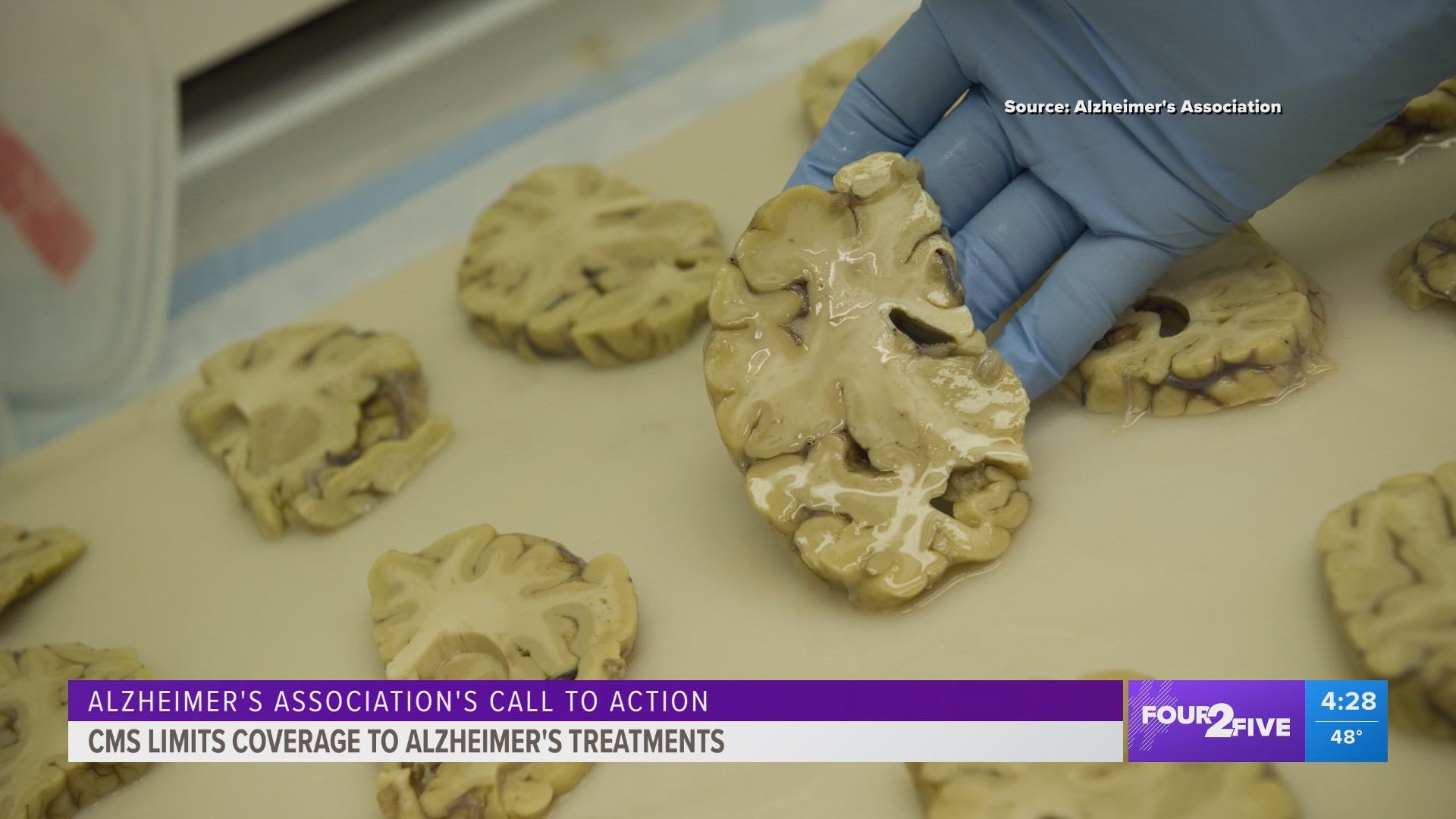
GREENSBORO, N.C. — The Alzheimer’s Association is speaking out after Medicare proposed to limit coverage of a new drug approved by the FDA to help Alzheimer’s patients. Aduhelm is the first Alzheimer’s drug approved by the FDA in the U.S. to slow cognitive decline. On January 11, the Centers for Medicare and Medicaid Services (CMS) released a draft decision stating it would only cover the drug for those participating in approved clinical trials.
Katherine Lambert is the CEO of the Alzheimer’s Association Western Carolina Chapter. She said this decision sharply limits access to treatment for many people living with the disease.
“Many of us do not live near a research institution,” Lambert said. “If you look at historic enrollment in clinical trials, this further exacerbates other health disparities. African Americans and Hispanics are at a greater risk for Alzheimer’s disease and are yet historically underrepresented in clinical trials.”
Lambert said denying people living with Alzheimer’s disease access to FDA-approved treatment is unacceptable and discrimination.
“It’s going to further by exacerbating these health inequities and honestly the entire disease,” Lambert said. “Individuals who have this diagnosis who have an FDA approved therapeutic should have access to that therapeutic. Just as you would with cancer, or HIV AIDS, or other health issues.”
The Alzheimer’s Association is calling on CMS to reverse its draft decision. There is a 30-day period for public comment after the draft decision is announced. The final decision will be announced by April 11.
The association is asking the public to learn more about this decision and add their voice on their website.