Julie's Story: From colon cancer diagnosis to her last chemo infusion
WFMY News 2's Julie Luck shares her treatment journey, her gratitude for those who reached out and encourages everyone to get screened.

"When you hear the word cancer, it's devastating. It's frightening. You just don't know what to expect," WFMY News 2 Anchor Julie Luck said.
She underwent a routine colonoscopy and was diagnosed with stage 3a colon cancer. She had surgery in late January. The hope was, that all the cancer was contained and the surgery would be it, but cancer had spread to her lymph nodes and chemo was ordered.

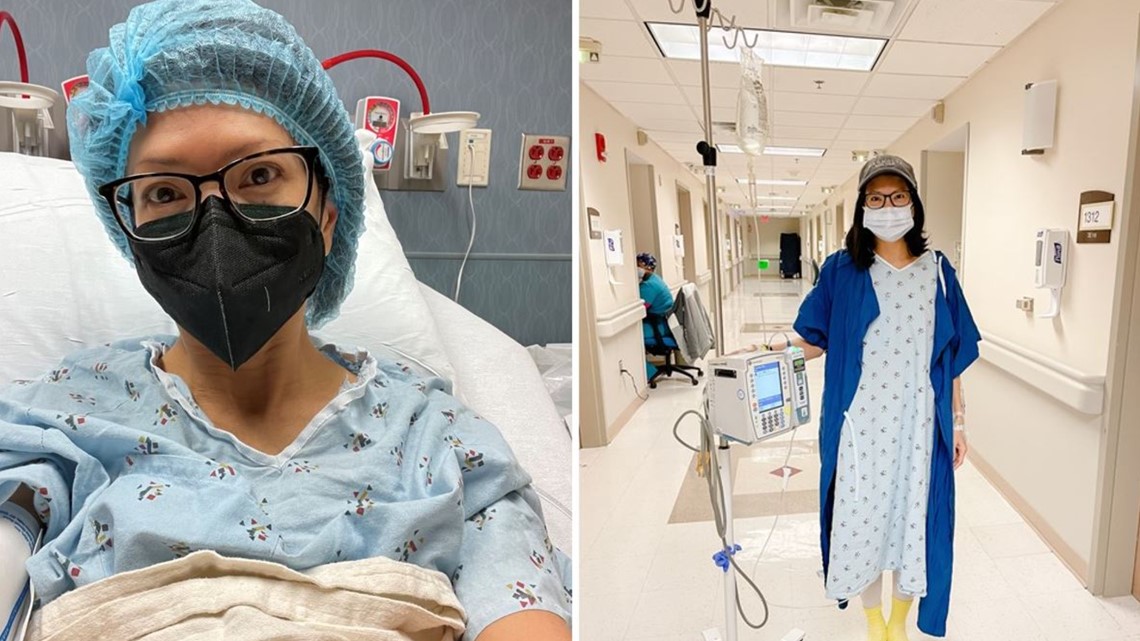
So far, there have been four chemo treatments. The actual treatment day is one thing. The impacts that come after are more than anyone wants to endure. Julie is sharing her story, her sickness, her pain, and her life-altering experience in the hopes you will get screened and avoid what she is enduring.
"If this is the catalyst, if this is the wake-up call, so be it. I'd like people to look at my situation and say, 'You know, this could be me,'" Julie said.
Chemo Infusions It's an All-Day Affair
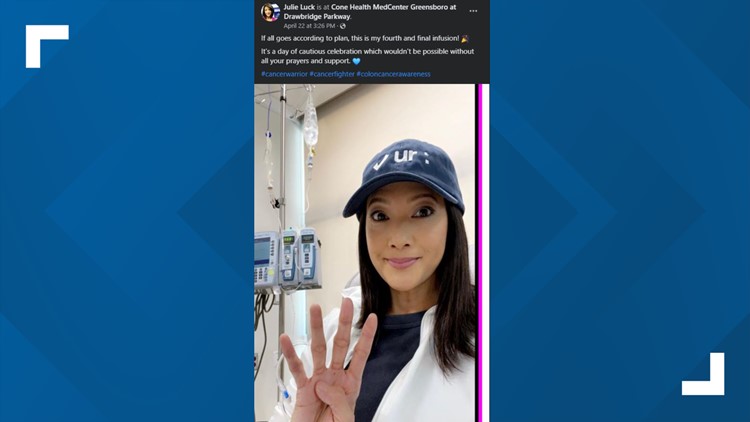
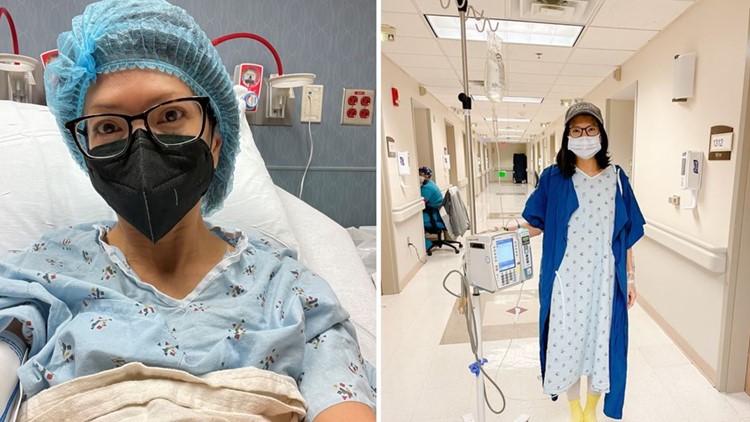
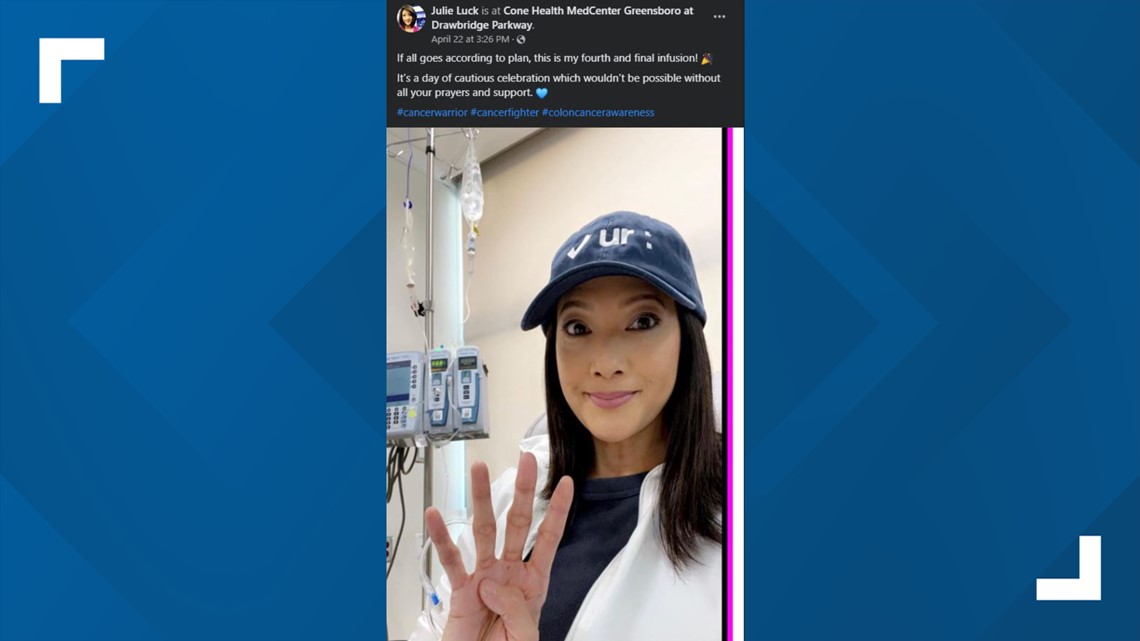
"It's the last one. I've been waiting for this day," said Julie as she raises her hands in the air.
Chemo infusion four was on April 22. Thankfully, the treatments have gone as planned with no delays, but that doesn't mean the treatment days are easy.

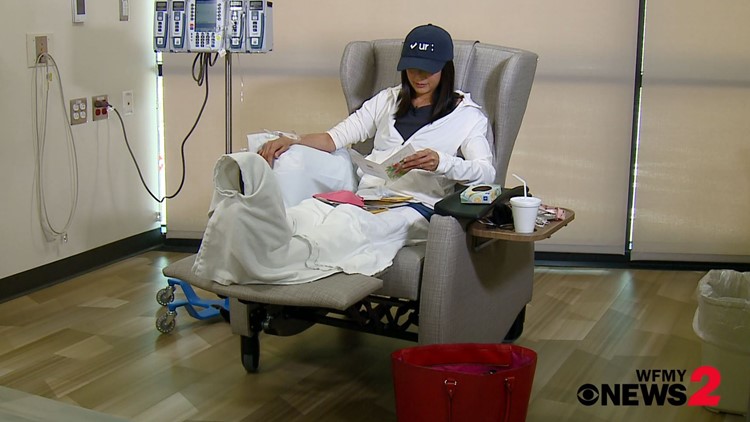
It's 11:45 a.m. on a Friday and Julie is already getting her vitals and blood work done. Then there's the waiting for tests to come back. Lots of waiting. If Julie's white blood count doesn't register at a certain limit, she can't go on with the infusion. A delay would be devastating.
"You're just taking it one day at a time. The prayers really are, 'just let this be the last one, let it be done. Let it be done. Let it be working the way it should,'" Julie said.
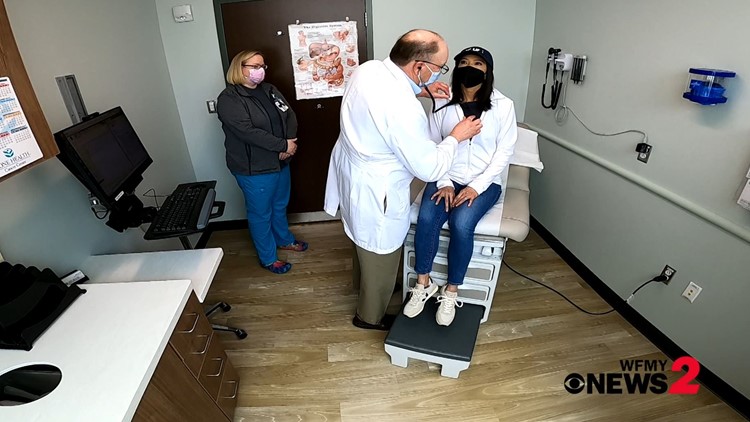
The doctor comes in to do more tests. He explains how the chemo makes the lines on her hands darker and that it should go away. He measures the numbness the chemo causes in her hands.
Now, it's 12:45 p.m. and time for the infusion process to begin. This process is what takes the longest time. It's several hours of chemo infusion, but before it can start, there are pre-meds to take by infusion.
Julie can rattle off the names of the drugs they're putting in the IV. They're words and terms she never thought she'd learn.
"I know way too much now; things I wish I didn't know," Julie said.


She never had symptoms of colon cancer, but now she feels the impacts of cancer. The infusion is just one of those impacts. She said chemo is lonely. Due to COVID, no one is allowed to visit with her while she gets the infusion. So, for hours, she sits in a chair, knowing the medicine being pumped into her is helping her and will also make her feel awful for at least the next 10 days.
Finally, around 5 p.m., she is out of the chair, ready to go home and deal with what comes next.


Warrior Fight Impacts and Side Effects of Cancer
Julie will tell you, that one of the worst side effects is nausea. She said it never really goes away. Waves upon waves of nausea, especially the first 10 days after each infusion. Yes, there are medications for nausea, but she will be quick to tell you that they barely touch it. Imagine, feeling like you're going to throw up 24/7, and yet you have to eat enough to keep nutrients in your body so that your blood work will be good enough to get your next infusion.
The first 10 days after an infusion are mostly spent sleeping, napping, and being quiet.
"The fatigue is ever-present. I'm a get-up-and-go girl, and I just can't," Julie said.
There's a long list of side effects she could have. Thankfully, she doesn't have all the ones on the list.
"The first thing people ask me is if I'm going to lose my hair. I'm not expected to with this kind of treatment," Julie said.
There are plenty of other impacts and side effects she does have. For example, a constant sour, metallic taste in her mouth. Because of it, she can only use plastic utensils, because if she uses a metal fork, it exacerbates that metallic taste.
"If I touch anything cold or cool, it feels like I'm getting small shocks of electricity," Julie said.
When we talk about it, she calls it 'the zaps.' Think about it, no touching the cold refrigerator door, or the sink handle to wash your hands. Not to mention, the zap the cold water would give you.
"If I drink anything cold or cool, it feels like there are shards of glass in my throat," Julie said.
She warms up orange juice in the microwave because she needs the nutrients to keep her white cell blood count up. She describes it as gross, but necessary.
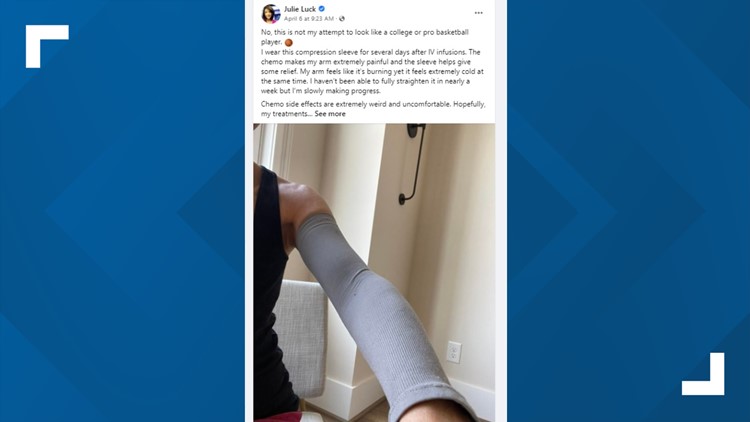
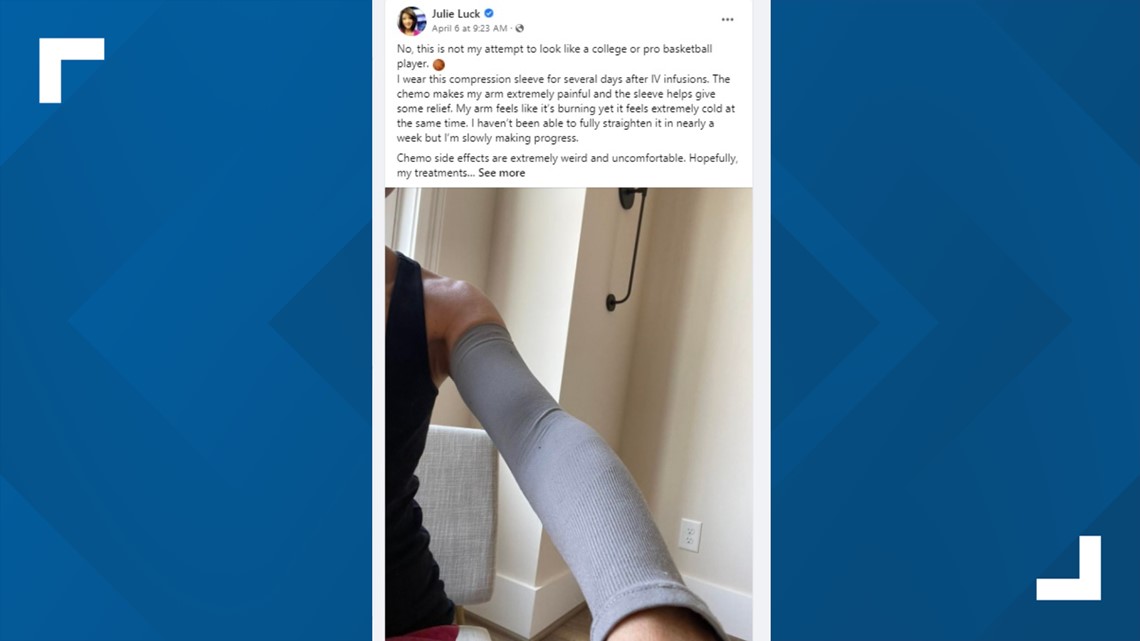
"After infusion, my arm is extremely sore for seven to 10 days, and wearing a compression sleeve helps alleviate some of the pain, so I kind of look like an NBA star," Julie said.
She jokes. She laughs. She has a sense of humor about it all, but make no mistake, this treatment has been excruciating.
"I'm tired of all of it. I just want this to be done," Julie said.

The Silent Army Praying The Cards and Well-Wishes
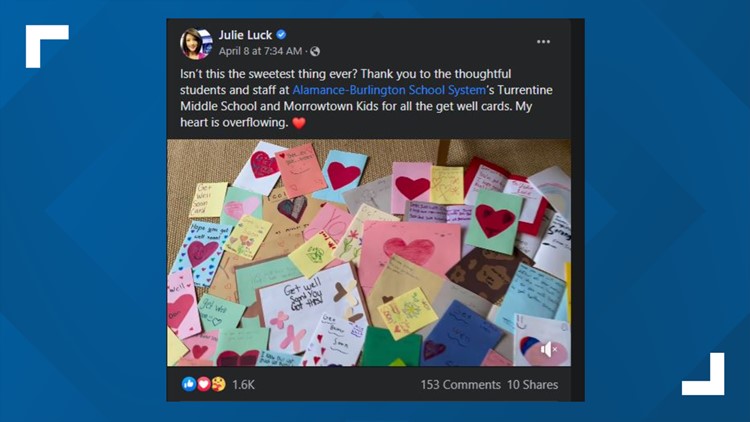
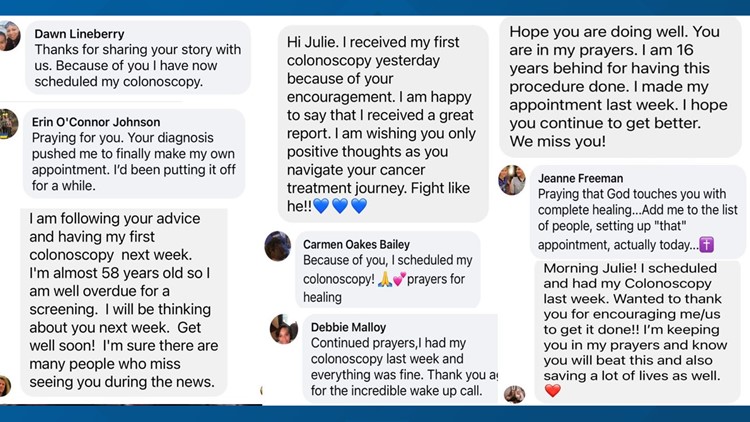
From the moment she told people on the air that she was diagnosed with colon cancer, the cards have flooded in.
"People at work will drop off the cards to my house, and these are stacks and stacks of cards," Julie said. "I read them and I'm always crying because they're so sweet, and for people to take the time out – people I've never even met – it’s so touching and I'm so grateful for it."


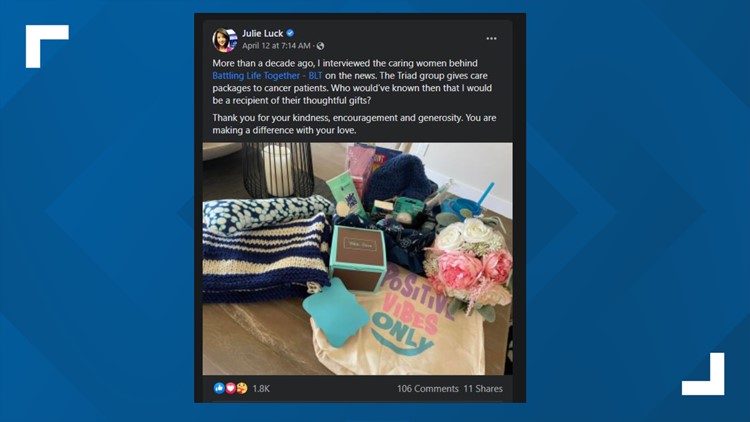
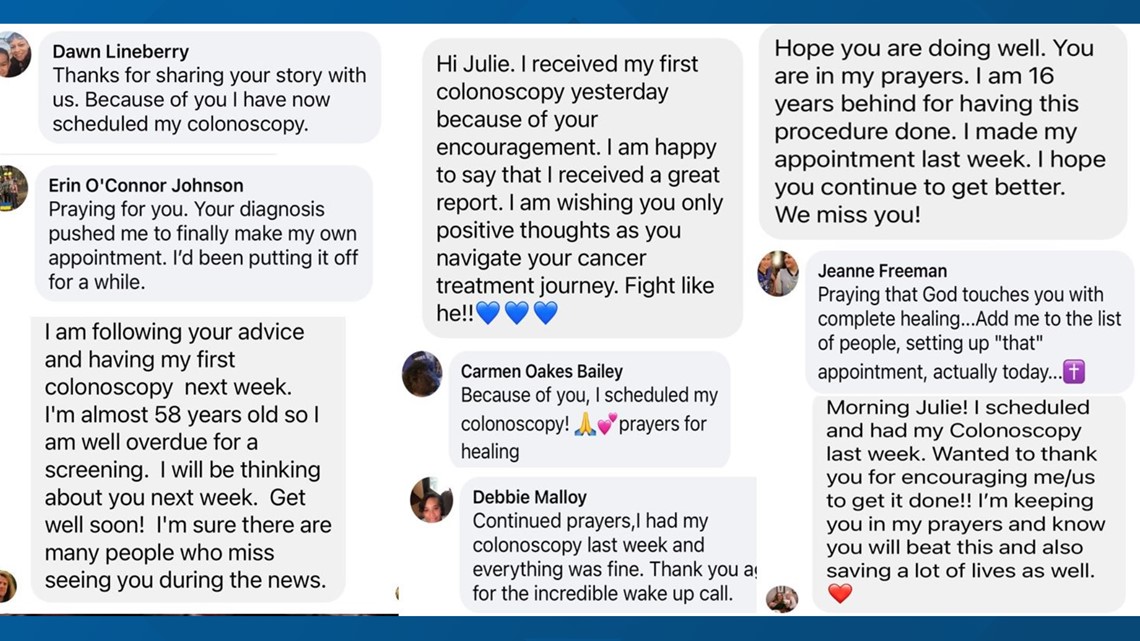
From cards to well-wishes on social media, emails, calls, texts, and gifts, Julie said she has an army of people who are watching over her, praying for her, encouraging her, and it is priceless.
"The positivity will get you through," Julie said. "I have this silent army, I might not see them, but I know they're there. Knowing people care to take the time has been awe-inspiring."
Don't Waste Your Cancer Check Your Colon
When Julie was diagnosed, it came as a shock, but immediately she knew she didn't want it to come as a shock to others.
"There's a saying, 'Don't waste your cancer.' That struck a chord with me," Julie said. "If I can encourage more people to get screenings, and those screenings save lives, that's me not wasting my cancer."

Julie got her first colonoscopy at 50 years old. She has no family history, she had no symptoms, she doesn't smoke, eats right, and exercises. There was no push to get screened earlier. Just recently, the age for screening was dropped to 45 years old. She wishes she had been screened then.
"I didn't know a screening or a colonoscopy could have prevented me from being in this situation. This is why I'm wearing this hat, check your colon," Julie said.
Her main focus, besides getting better, is to get the word out. Everyone needs to be screened for colon cancer, regardless of how good they feel.
"Life takes over, I get it, but you can take one day and get it done," Julie said. "Think of all the time it takes for me to come here, undergo surgery, the heartache and pain emotionally and physically. It has been taxing."


What's Next? Hope For Tomorrow and Beyond
Julie calls herself "cautiously optimistic." She's hoping no more treatments need to be done. She will have another round of blood tests before she can ring that cancer-free bell. Later this year, she will have a CT scan to confirm the cancer is gone and the treatments have worked.
Julie's Journey: Battling colon cancer and raising awareness
Colon Cancer Risks and Symptoms
In 2022, an estimated 151,030 people will be diagnosed with this highly preventable disease. They will join more than 1.4 million colorectal cancer patients and survivors living today.
However, more than 50,000 Americans die each year from colorectal cancer, and the number is growing rapidly for those younger than 50, according to the Colorectal Cancer Alliance.
Here are three things to know about colon cancer, including who’s at risk, symptoms, and other risk factors.
1. People most at-risk for getting colon cancer:
- Anyone with a family history
- Someone with irritable bowel syndrome
- African Americans have a 20% increased risk over white people
2. Risk factors for colon cancer:
- Smoking
- Drinking
- Obesity
- Diet high in red meat
- Diet low in fruits and vegetables
3. Symptoms of colon cancer:
- Persistent change in bowel habits
- Diarrhea
- Constipation
- Blood in stool
- Abdominal pain
- Discomfort
- Cramps
Take a short quiz to learn more about which screening options are best for you based on your personal risk factors.
If you have questions about specific screening tests, who should be screened and when, or anything else related to colon cancer screening, we encourage you to talk with your doctor or call the toll-free helpline at (877) 422-2030.
Find out more resources about colon screenings.
RELATED: Colon cancer support group | Join the conversation as dozens of people share their experience